How Do Pharmaceutical Companies Test New Drugs?
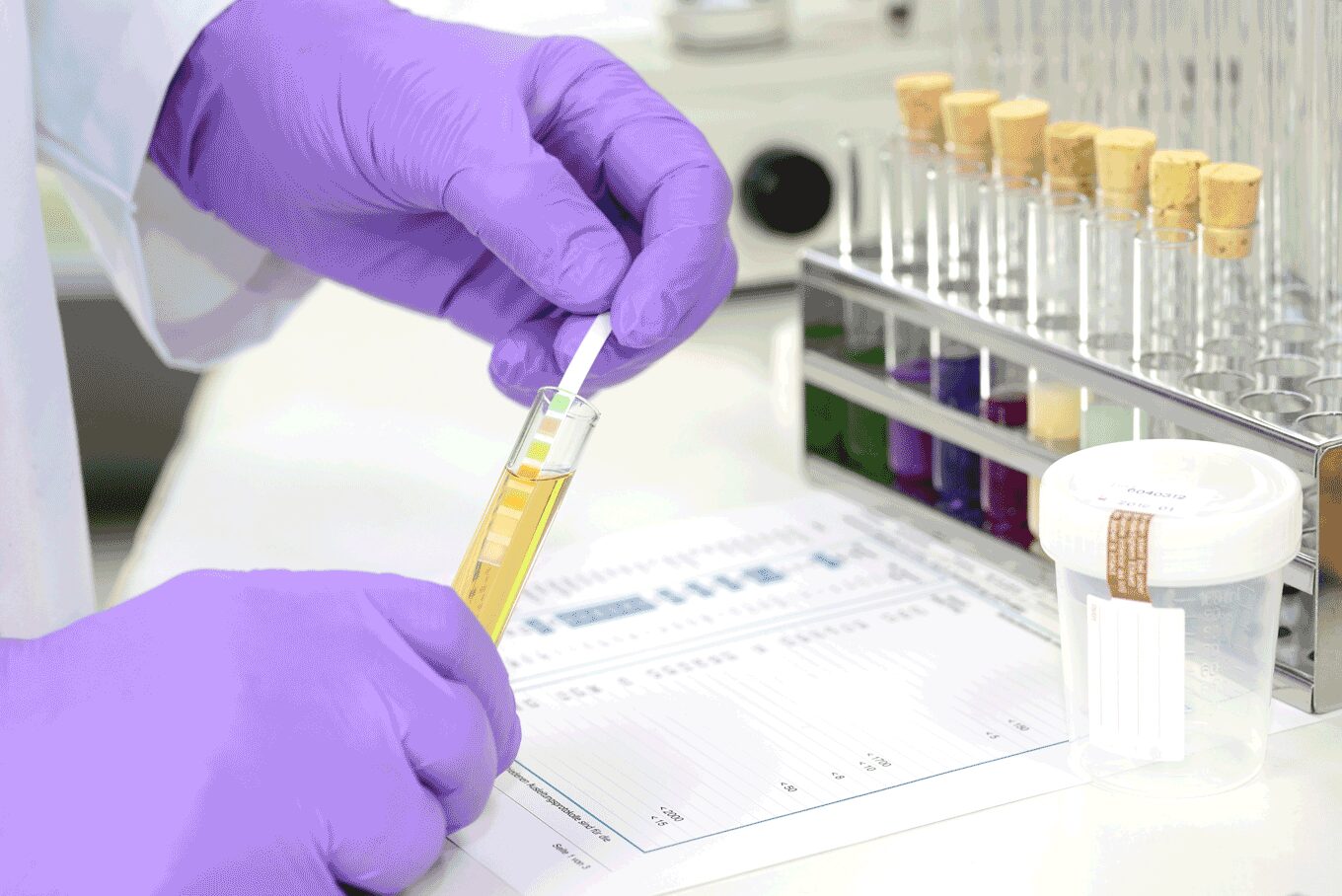
Drug safety assessment belongs to the most important ethical issues addressed by pharmacology and medicine in general. Drug safety is a significant outcome of all phases of testing, even non-interventional testing.
While there are typically around 50 or so new drugs licensed for use every year, tens of thousands of candidate drugs never make it. Pharmaceutical companies like AdarePharmaSolutions embark on a long and expensive journey to get a new medication to the market.
Every drug that can be prescribed around the world has been approved by national regulatory authorities, like the European Medicines Agency (EMA), the U.S. Food and Drug Administration (FDA), and the Australian Therapeutic Goods Administration (TGA). Approval only comes after the drug has completed every stage of the required clinical trials. Clinical trials are an important part of drug development globally, with some of the latest figures available revealing nearly 43 percent were made up of U.S. participants. These trials have grown more complex in recent years and are vital for the research and development of new drugs.
A pharmaceutical company seeking FDA approval for a new drug must complete a process that includes the discovery and development stage, preclinical research, clinical research, and FDA review. And, it doesn’t end there as the FDA continues to monitor its safety post-market too.
Discovery and Development Phase
There may be thousands of compounds that are potential candidates for development as medical treatments, but after early testing, just a small number appear promising enough to call for further study. This is the first step in the testing process, with experiments conducted on those who make it through to determine the potential benefits, how it will best be administered, optimal dosage, side effects or adverse events, how it affects various demographics such as a particular race or gender, and how it interacts with other treatments and medications.
Preclinical Research
Before a drug can be tested in humans, researchers must determine whether it has the potential to cause toxicity or serious harm. There are strict regulations setting out the minimum requirements by the FDA, from personnel to facilities and equipment. Typically, the preclinical studies aren’t large, but they must provide detailed information on toxicity and dosing levels for researchers to decide whether a drug should be tested in people.
Clinical Research

The next phase of testing refers to the clinical trials or studies that are conducted on people. They must be efficacious and safe, completed under the drug development budget while using a methodology that ensures the drug works for its intended purpose as well as possible. It’s a rigorous process that requires many volunteers who have the condition the new drug is meant to treat. The trials in this phase can last for several years to thoroughly evaluate how the medication works in comparison to other medications already on the market for the same condition. It must be deemed by investigators as at least as safe and effective as other treatments that exist.
FDA Review
If a developer of a drug has evidence from all previous phases that it’s safe and effective, the company can then submit an application to the FDA for approval to market the drug. The FDA review team will thoroughly examine all the data on the drug to decide on whether to approve or decline. Once the drug is approved by the FDA, there are more clinical trials involving thousands of volunteers that can last for many years. This phase provides even more information about the drug’s effectiveness and long-term safety.
Animal experiments

Although for many the first association is animal testing, it is true that these studies and tests have yielded very poor results in most cases. Many of the most important health advances are due to human studies, including anesthesia; bacteriology; microbial theory; stethoscope; morphine; radium; penicillin; artificial lungs; antiseptics; scanning; the discovery of a link between cholesterol and heart disease and between smoking and cancer; X-ray detection; and isolating the virus that causes AIDS. Animal testing played no role in these and many other discoveries. Due to physiological differences between humans and other animals, the results obtained from animal tests cannot be mapped identically to humans, leaving us vulnerable to drug exposure, which can cause serious side effects. Of course, we must not forget that many of the procedures we have today have been developed on animals, such as the polio vaccine.
Who are the participants in clinical researches?
The persons over whom clinical trials are conducted are mostly patients who are for trials find out through their specialist doctors. After being selected according to the clinical trial plan, the respondents get acquainted with the main researcher information on an oral clinical trial and
in writing. Respondents receive a document (Informed Consent) explaining the details of the clinical trial and their role in them. No respondents are included in a clinical trial if not signed voluntarily consent.
What are the risks of participating in clinical research?
The risks of participating in a clinical trial include ineffectiveness and adverse drug reactions that examine those risks associated with the procedures being conducted in the examination. Respondents are before the start participation in the examination introduces all known risks. Before approving the examination by the Agency assesses the justification and acceptability of the risk for respondents.
Final thoughts
Clinical trials are scientific and medical trials that are conducted on healthy or sick volunteers who gave consent to participate. Clinical trials collect data on efficacy and the safety of the use of drugs, medical devices, diagnostic methods, disease prevention methods, medical procedures (eg surgical procedures), or methods of treatment. New drugs are being tested, but also already approved ones, which can be tested in additional indications (for other diseases), in new forms, in special subgroups of patients, and similar. Clinical trials are conducted according to a predetermined test plan (protocol), in accordance with a number of international regulations, conventions and guidelines, and laws and regulations in the country in which they are conducted. The main principles of conducting any clinical trial are protection the rights, security, and confidentiality of respondents’ data and the accuracy and reliability of the results, which is ensured by comprehensive mechanisms to ensure control, monitoring, supervision, and inspections.




